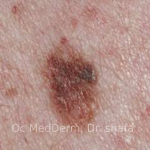
Always benign
between benign and cancer
Deadly cancer
An atypical mole is a strange-looking mole whose appearance is not round and clean like a common mole, but also not ugly looking like melanoma, a deadly skin cancer. Atypical moles clinically, as well as histologically (under microscope), fit between common mole and melanoma. They are not cancerous yet but have a higher potential to grow into melanoma.
Beside increased lifetime sun exposure and being from melanoma prone families, the number of atypical moles increases the risk of melanoma. People who have atypical moles are at increased risk of developing melanoma in a mole or elsewhere on the body. Those who have 10 or more atypical moles have 12 times the risk of developing melanoma compared with the general population.
Individuals with AMS, medically called Dysplastic Nevus syndrome (DNS), are people with more than 50 moles, with three or more moles atypical in shape, size, structure, or color. People with AMS are at higher risk ( 7 to 10 fold) of developing melanoma.
“Atypical Moles” have the potential to grow to a deadly skin cancer called “Melanoma”. If you find that one of your existing moles is changing or you developed a weird-looking mole, call us for an appointment to have your moles checked. During your medical visit, Dr. Shafa will evaluate your suspicious mole with a handheld skin microscope called “Dermoscope”. Any suspicious criteria under a dermoscope justifies a biopsy of an atypical mole to rule out skin cancer.
We know that common moles are safe and benign, and that melanoma is an aggressive deadly skin cancer. Atypical moles clinically and microscopically fit in between common moles and melanoma. Their behavior is unknown and unpredictable, as they can remain unchanged or grow into melanoma.
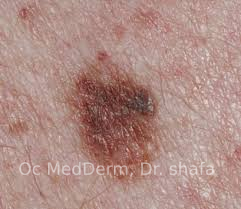
An atypical mole also called “dysplastic nevus” can look like fridge eggs.
Flat or slightly raised, it can have irregular borders and is generally larger in size (6-12 millimeters) than ordinary moles. Their color is oftentimes not uniform and varies from tan to dark brown.
Yes. Heredity appears to play a part in the formation of atypical moles. They tend to run in families, especially in Caucasians; about 2 to 8 percent of Caucasians have these moles.
The existence of atypical moles and family history for melanoma increases the risk of having such skin cancer. Therefore Dr. Shafa recommends once or twice a year skin check with a dermoscope if you are at high risk.
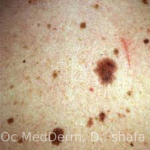
If you have an unusual, atypical-looking mole, be educated about its appearance of skin cancer and detect it early. If your mole is changing, has a ‘funny look,” or you’re concerned and your gut feeling says something is wrong, just give us a call and let us check it under a dermoscope or perform a quick procedure called a “skin biopsy”.
If you are suspicious of any mole, do not hesitate to make an appointment with Dr. Shafa for an evaluation. A mole biopsy is a very simple and pain-free procedure that takes no more than a few minutes. It is always worth it to be on the safe side.
Although an individual mole is unlikely to become malignant, the single best predictor of risk for the development of melanoma is the total number of moles.
No. Moles are extremely common and numerous, therefore, preventative removal of moles is not justifiable. However; a mole should be biopsied and examined microscopically if it has any of the characteristics of concern (ABCDE of melanoma).
No. The specimen must be deep enough for an accurate microscopic diagnosis and should contain the entire lesion if possible, especially if the concern for malignancy is high. However, wide primary excision is not needed initially even for highly abnormal-appearing lesions, because many such lesions are not cancerous.
No. A skin biopsy, even one that involves cutting through skin cancer, does not increase the likelihood of cancer spreading (metastasis). Dr. Shafa uses her expertise during mole removal to avoid extensive surgery for a skin lesion, yet she ensures that she has removed a sufficient amount of tissue for efficient microscopic evaluation of the entire mole. Of course, Dr. Shafa’s artistic touch also ensures the best cosmetic outcome as well.
Other Treatments
Why Choose Us for Your Skin Surgery | Mole Overview | Typical Moles | How We Remove Moles | Other Skin Lesions That Might Look Like Moles | Mole Gallery
Book a consultation at OC Medderm | Irvineskin Today for Medical, Surgical, and Cosmetic Dermatology in Irvine & Orange County, CA.
We are experts in Acne, Pinch blepharoplasty, Ear lobe repair, Xanthelasma repair, Syringomas removal, mole removal, Keloid removal, Body and face piecing or piercing repair or removal, lump and bumps removal, Acne scar removal, Spider vein treatment, fungal infection, Co2 resurfacing, Warts and more.
You can schedule an appointment or call us now for all the dermatology treatments. We are located at 113 Waterworks Way 100, Irvine, Orange County CA, We Are Dedicated to Providing the Best & Transparent Dermatology Care for your skin.
Call us when you want!